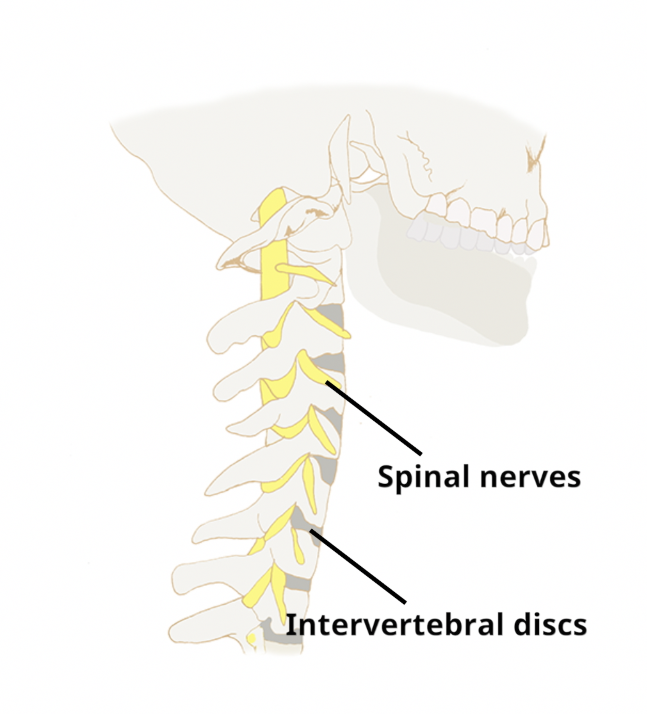
Acute neck pain is the medical term used for the intense neck pain which some individuals may experience.
Studies have shown that many people will suffer with at least one significant episode of neck pain at some point in their adult life.
There can be many causes for acute neck pain. However, the intense pain, stiffness and locked feeling that individuals may experience is often the result of muscle spasm rather than being directly related to the extent of injury to a disc or surrounding tissues.
If you are experiencing any pins and needles or numbness in the face or arm, we would recommend that you seek medical assessment.
How is acute neck pain treated
Acute phase management
Acute phase management is aimed at alleviating pain to allow rehabilitation to commence as early as possible following injury.
Ongoing management
Exercises
Specific exercises to relieve any stiffness in the neck & upper spine and maintain flexibility at the shoulders.
Using painkillers when needed
Over-the-counter analgesia is available through pharmacies when needed. Paracetamol is most commonly prescribed. Anti-inflammatories, such as Ibuprofen, are also used, but as there is little or no inflammation involved in osteoarthritis these are best avoided without discussing with your GP. Side effects are even more common than with paracetamol so please ensure to take appropriate medical advice. There is a good booklet on the Versus Arthritis website with information about the various drug options: Painkillers and NSAIDs | Side-effects, uses, time to work (versusarthritis.org)
Modifying ergonomics
Modifications include raising your seat height, changing the backrest angle, lumbar wedges as well as ensuring there is an appropriate overall set up if working with display screen equipment. Everyone is different so try out slightly different combinations which may work best for you.